|
|
CPAP
CPAP (Continuous positive airway pressure) therapy
for Obstructive Sleep Apnoea (OSA)
Continuous positive airway pressure therapy
(CPAP) uses a machine to help a person who has obstructive
sleep apnoea (OSA) breathe more easily during sleep.
A CPAP machine increases air pressure in your throat
so that your airway does not collapse when you breathe
in. When you use CPAP, your bed partner may sleep
better, too.
CPAP Machines
-->
You use CPAP at home every night while you sleep.
The CPAP machine will have one of the following:
• A fullface mask that covers your nose and mouth.
• A nasal mask that covers your nose only-called
nasal continuous positive airway pressure, or NCPAP
(this type of mask is most common).
• A pillow mask that fits into your nose. |
| |
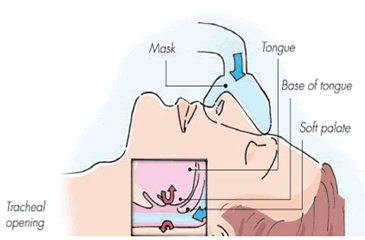
If you have been diagnosed with obstructive sleep
apnoea (OSA), a condition in which relaxation of the
muscles around the tongue and throat causes the
tissues to block airflow to the lungs while you
sleep, CPAP therapy is the recommended form of treatment for those individuals who suffer from sleep apnoea.
Benefits of CPAP include keeping your airways open
while you sleep, easing snoring, improving sleep
quality, relieving daytime sleepiness, and lowering
blood pressure.
Although you will likely feel better rested and
alert once you start CPAP, getting used to the device
can take some time. Some people have difficulty
sleeping the first few nights of treatment. |
|
 |
| |
|
|
You may want
to try an Auto CPAP machines that have automatically
adjustable air pressure or air pressures that are
different when you breathe in than when you breathe
out.
What To Expect After Treatment
It may take time for you to become comfortable with
using CPAP. If you cannot get used to it, talk to
your doctor. You might be able to try another type
of mask or make other adjustments.
Why It Is Done
CPAP is the most effective nonsurgical treatment
for obstructive sleep apnea. It is the first treatment
choice and the most widely used.
• Doctors use CPAP to
treat people who have moderate to severe sleep apnoea.
• CPAP is the treatment of choice for people
who have sleep apnoea and coronary artery disease
(CAD) or heart failure.
How Well It Works
Overall, CPAP is the most effective treatment for moderate and severe
obstructive sleep apnea:
• Research shows that continuous positive
airway pressure (CPAP) decreases daytime sleepiness,
especially in those with moderate to severe sleep
apnea..
• Studies show that in people who have moderate
to severe sleep apnea, nasal continuous positive
airway pressure (NCPAP) lowers blood pressure during
both the day and the night.
• CPAP is often more effective than other non-surgical methods
for treating systemic obstructive sleep apnea.
• People with coronary artery disease who
use CPAP for sleep apnea are less likely to have
heart problems such as heart failure. |
| |
Problems that may occur with CPAP include:
• Dry nose and sore throat.
• Nasal congestion, runny nose, and sneezing.
• Irritation of the eyes and the skin on the
face.
• Abdominal bloating.
• Leaks around the mask because it does not
fit properly.
Nosebleeds are a rare complication of CPAP.
You can expect mild discomfort in the morning when
you first start using CPAP. Talk with your doctor
if you do not feel comfortable after a few days.
Relieving side effects
You may be able to limit or stop the side
effects: |
|
 |
• Your doctor may be able to adjust your CPAP
to reduce or eliminate problems.
• Be sure the mask or nasal prongs fit you
properly. Air should not leak around the mask.
• Use a humidifier or a corticosteroid nasal
spray medicine to reduce nasal irritation and drainage.
• You may want to talk to your doctor about
trying a CPAP machine that will start with a low
air pressure and slowly increase the air pressure
as you fall asleep. This kind of machine can help
reduce discomfort caused by too much constant pressure
in your nose. If this does not improve your discomfort,
ask your doctor about trying a bilevel positive
airway pressure machine (BiPAP), which uses a different
air pressure when you breathe in than when you breathe
out. BiPAP may work better than standard CPAP for
treating obstructive sleep apnea in people who have
heart failure. BiPAP machines are more expensive
than CPAP machines.
• If your nose is runny or congested, talk
with your doctor about using decongestants or corticosteroid
nasal spray medicines or fullface masks.
What To Think About
When you are using CPAP, you need to see your doctor
or sleep specialist regularly. You may also need
more sleep studies to adjust the CPAP machine and
check whether the treatment is working.
The most common problem with CPAP is that people
do not use the machine every night. Or they take
off the mask during the night because it becomes
uncomfortable. Even one night of not using the machine
can make you sleepy the next day.
You might not use the machine daily, or you might
even stop using it because:
• You don't like wearing a mask because of
nasal discomfort.
• The machine is noisy.
• It may discourage intimacy with your sleeping
partner, even though you use the machine only while
you are sleeping.
The best treatment for obstructive sleep apnea depends
on a number of factors, including the severity of
your problem, the physical structure of your upper
airway, other medical problems you may have, as
well as your personal preference. You should work
with your doctor or sleep specialist to select the
best treatment option for you.
CPAP
Machines --> |
| |
Snoring Treatments & Solutions
If you occasionally snore, you
can try the following conservative behaviour changes to help treat
the problem:
• Lose weight and improve your eating habits.
• Avoid tranquilizers, sleeping pills, and
antihistamines before you go to bed.
• Avoid alcohol, heavy meals, or snacks at
least four hours before you sleep.
• Establish regular sleeping patterns. For
example, try to go to bed at the same time every
night.
• Sleep on your side rather than on your back.
• Prop the head of your bed -- not just your
pillows -- up four inches.
If none of the above mentioned behavioural changes
help snoring, talk to your doctor. Otolaryngologists
(ear, nose, and throat doctors) offer a variety
of treatment options that may reduce or eliminate
snoring or sleep apnea.
There are more than 300 devices on the market to
help prevent snoring; however, none of these devices
address all of the underlying anatomical problems
that cause snoring (such as nasal obstruction and
being overweight). Surgery may be one option needed to correct
physical problems.
Snoring and Sleep Apnoea Surgeries
Uvulopalatopharyngoplasty (UPPP or UP3): A surgical treatment that tightens and restructures
the flabby tissues in the throat and palate. This
is often prescribed for people who have moderate
or severe obstructive sleep apnea.
Laser-assisted uvula palatoplasty (LAUP): A laser procedure removes the airway obstruction.
This treatment is performed under local anaesthesia
in a doctor's office and is intended for snorers
and for people with mild obstructive sleep apnea.
Somnoplasty: This is a minimally
invasive procedure that uses radio frequency energy
to shrink excessive tissue in the palate, uvula,
and tongue tissue. This treatment can also be used
to relieve nasal obstruction.
Genioglossus and hyoid advancement: This is a surgical treatment for sleep apnea which
prevents the collapse of the lower throat by pulling
the tongue forward.
Septoplasty and turbinate surgery: This is a surgery to fix blockages in the nose and
help air through the nose smoothly and quietly.
Tonsillectomy: Removing the tonsils
and adenoids may be needed to prevent snoring, particularly
in children.
|
|
|